Note: This topic intersects a little with my day job, so it’s a good time to remind you that the opinions here are mine alone.
The wealthy world’s physicians are getting older as part of the broad demographic shift we’re undergoing. People in many high-stakes professions face mandatory retirement or restrictions on their activities as they age: everyone from judges to airplane pilots to FBI agents has to end their career at an age when their potential for cognitive decline poses a risk to public safety. Arguably, physicians have a similar impact on public safety, but are generally allowed to continue practicing as long as they like, barring obvious loss of mental fitness.
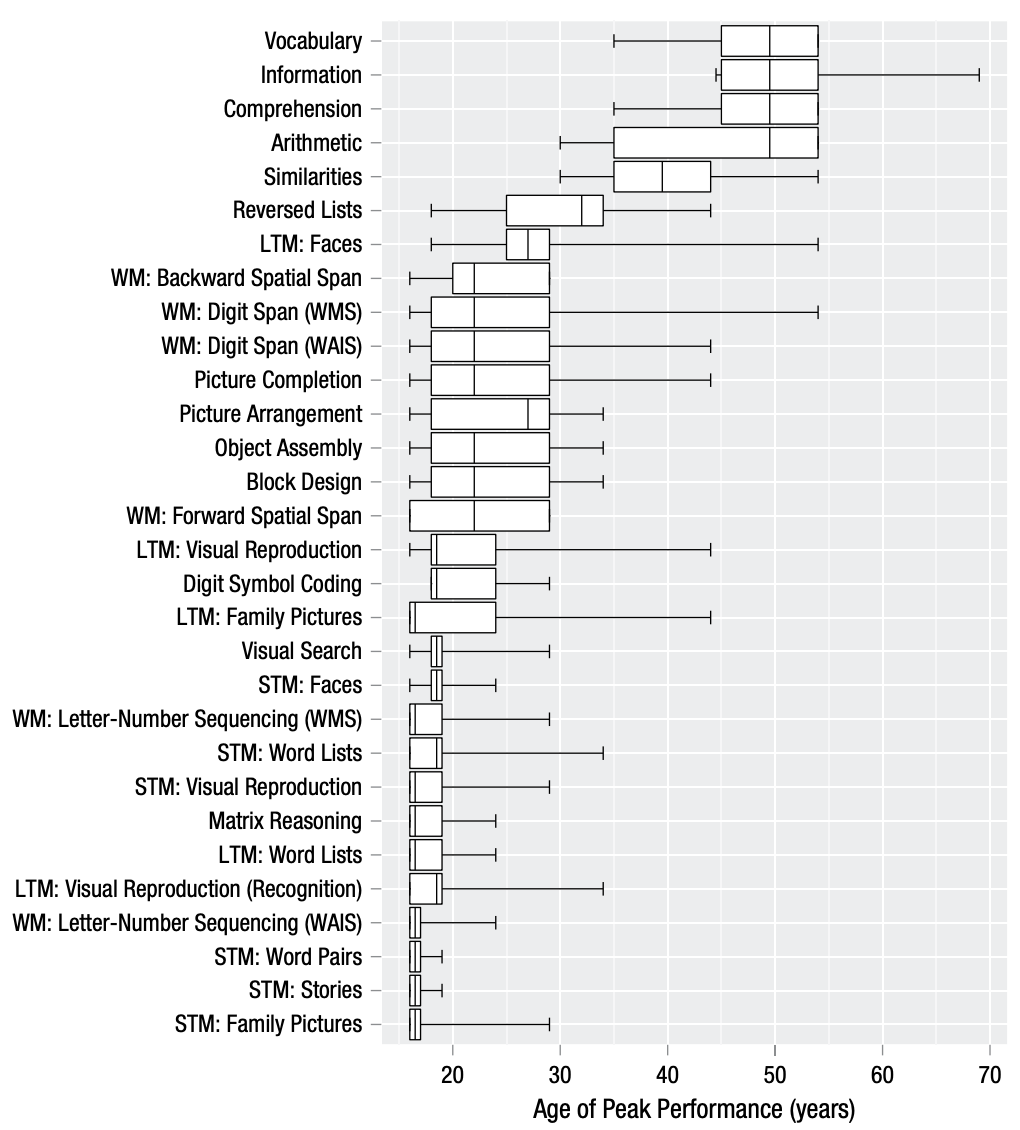
It’s extremely expensive to train new physicians, and the public bears much of that cost. Given this cost and the ever-present shortage of physicians, we should be thankful in a way for physicians who extend their careers past the usual retirement age. At the same time, many of our cognitive abilities peak before we’re 30. Most physicians don’t even finish their training until after that age, though, and the potential decline of cognitive faculties that often accompanies aging might pose a risk to patients.
I wanted to see what evidence is out there on how physician ability changes with age and where the differences in ability come from. I was curious too what factors might mitigate any risks to safety posed by physician aging.
Outcomes
The strongest signal of physician ability is how their patients do, and there’s no less ambiguous indicator of that than mortality. It can be difficult to actually get that signal, so many studies work with intermediate measures like tests of medical knowledge or adherence to guidelines. To me, these are potentially useful for explaining the findings of studies that capture patient outcomes, but they don’t provide a useful signal on their own.
Big, well-powered studies like this are relatively rare. Among non-surgeons, I’ve found just four:
Norcini (2000): Certification and specialization: Do they matter in the outcome of acute myocardial infarction? In short, yes, and so does physician age. This study looked at mortality in a group of 40,684 patients hospitalized after a heart attack in Pennsylvania in 1993. These patients were treated by a total of 4,546 physicians. After adjustment for a range of risk factors, the researchers found that mortality increased 0.5% for each year the physician had been out of medical school (which is correlated with age, of course).
Norcini (2017): Patients of doctors further from medical school graduation have poorer outcomes. This study, again from Pennsylvania, looked at outcomes in 694,020 hospitalizations managed by 5,280 physicians between 2003 and 2009 for one of five conditions: acute myocardial infarction, congestive heart failure, gastrointestinal hemorrhage, hip fracture, or pneumonia. Adjusted mortality rates were again found to be elevated among more experienced physicians — here, they increased by about 0.45% per year. Across the five conditions, the additional risk from being treated by an older physician was relatively stable, but topped out at about 0.6% per year for gastrointestinal hemorrhage.
Tsugawa (2017): Physician age and outcomes in elderly patients in hospital in the US: observational study. These researchers examined a sample of 2011-2014 Medicare data on the outcomes of 737,537 hospitalizations of elderly people associated with 18,854 physicians. They adjusted for a huge range of potential confounders and discovered that patients treated by a physician below age 40 were 11% less likely to die within 30 days of hospitalization compared to patients treated by physicians aged 60+.
Miyakawi (2023): Association between emergency physician’s age and mortality of Medicare patients aged 65 to 89 years after emergency department visit. This study shares several authors with the previous one and shares much of its methodology too. Instead of focusing on all inpatient encounters, it focuses on elderly patients seen in the emergency department. Among 2,629,464 encounters managed by 32,570 physicians, they found that adjusted 7-day mortality was 11% higher among physicians aged 60+ compared to physicians younger than 40.
These studies are, I’d say, remarkably consistent in the directionality and even the effect size. All of them say that being treated by a physician older than 60 versus a physician under 40 carries about a 10% increase in mortality risk across a broad range of conditions treated in hospitals. When we look at the absolute difference in mortality rates, that translates into a pretty shocking statistic. Using absolute mortality rates from the Tsugawa paper — 10.8% for physicians <40 and 12.1% for physicians 60+ — we find evidence that 1 in 77 elderly people treated by a 60+ year old physician in an inpatient setting dies because they were not treated by a younger physician.1 That number drops to 1 in 500 for the Miyakawi paper, although they use 7-day instead of 30-day mortality. Either way, these are awful numbers.
A little nuance
The Norcini papers are not as well-done as the others. It’s not clear whether the first of his papers excludes physicians in residency, who benefit from a lot more supervision, although the later one does. The bigger issue is that physician age is treated as a linear variable — that is, Norcini assumes in these analyses that every additional year will have the same amount of impact on patient outcomes, no matter the age you’re comparing it to. The other papers allow for non-linear relationships between physician age and outcomes. This turns out to be a solid design choice, as seen in the following chart from the Tsugawa paper. Most of the increase in risk happens after age 60, meaning that Norcini’s studies treating age as a linear variable would likely overestimate mortality attributed to middle-aged physicians and underestimate mortality attributable to older ones.
All of the papers point to factors that can offset the risk of treatment by an older physician. The Norcini papers point to board certification as a way to mitigate the risk of aging. Specifically, board certification offsets about 15 years of aging, presumably by keeping clinical knowledge more up to date. To get a sense of how that would impact mortality, Norcini writes, “we calculated what would have happened if certified doctors had treated all of the study’s approximately 30,000 hospitalized [acute myocardial infarction] patients. We estimate that 481 fewer in-hospital deaths could be expected when compared with treatment of all patients by non-certified physicians.” For treatment of heart attack, the same paper also says you’re also better off having a cardiologist of any age than an internist or family physician — he writes that 802 fewer in-hospital deaths would have taken place if cardiologists had treated them all. This effect would be magnified further if you looked only at board-certified cardiologists. Interestingly, the 2017 Norcini paper also finds a huge effect of immigrant physicians: non-citizens who went to a non-US medical school had mortality rates matching US medical school graduates 20 years younger.
Tsugawa, meanwhile, finds that the primary way of offsetting physician aging is through high patient volumes. When examining physicians in the top third of patient volumes, there were no significant differences in mortality between physicians aged <40 and those aged 60+.2 Among physicians in the lowest third of patient volume, there’s a whopping 34% increase in mortality among the oldest group of physicians compared to the youngest — equivalent to 1 in 23 elderly people treated by an older physician in this low-volume group dying because they weren’t treated by a younger doctor. In the medium-volume group, it’d be 1 in 59. Thankfully, the high-volume group is responsible for about two-thirds of the admissions in this study, so the actual quantity of excess deaths is lower than it might be. Still, if we take these numbers seriously — and I think the Tsugawa study is well-done enough to merit taking seriously — they should give us pause.
Curiously, the 2000 Norcini paper found a substantial decrease in mortality risk among physicians with high volumes that wasn’t replicated in either his 2017 paper or in Miyakawa’s. There was, though, a minuscule protective effect among high-volume facilities (but, again, not high-volume physicians) in the 2017 Norcini study.
I’d like to briefly touch on whether this research translates to surgeons. There is evidence that patient volume plays a role in improving outcomes for older surgeons. But otherwise, the lessons from the studies of non-surgeons don’t cleanly generalize to surgeons. A Canadian study containing patient outcome records of 3,314 surgeons found a 5% decrease in mortality for each decade of a surgeon’s age, while at the same time suggesting that age has a variable effect by surgeon specialty. Among vascular and plastic surgeons, age seems to be very advantageous, while it’s slightly disadvantageous for gynecological and urological surgeons. Ultimately, surgeons use a different cognitive skillset from most other physicians, so it makes sense that there might be a different relationship between age and ability for them.
Is this attributable to different patient types?
It’s possible that more experienced physicians deal with more complex patients whose mortality risk is poorly captured in the adjustment variables. All the studies attempt to control for individual patients’ baseline mortality risk, but this can always fail. From the studies themselves, you do see some signs of imbalance across physician types: Tsugawa finds that older physicians tend to treat patients with a significant but tiny increase in the comorbidity count of patients; and the mortality prediction used in the 2000 Norcini paper is less accurate than we might hope. Strangely, the 2000 Norcini paper also finds that rural hospitals are associated with lower adjusted mortality. Most patients in rural locations with more severe illness would be transferred to a larger facility, which suggests to me that disease severity wasn’t fully captured in the variables they used and is spilling over onto the location variable.
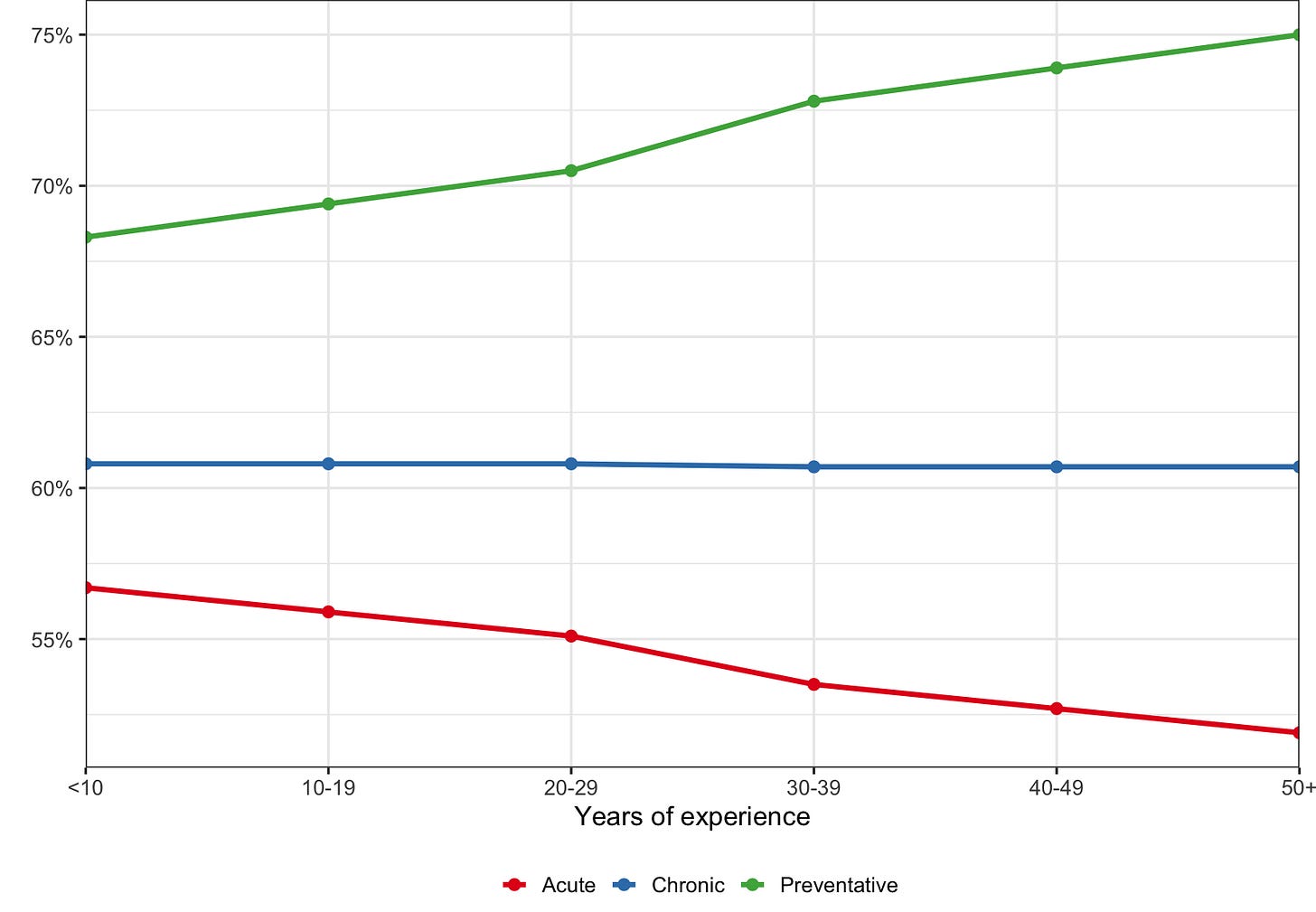
More broadly, there’s evidence that older physicians perhaps should treat different patients, since they might be better at providing some types of care than others. Orler, et al. (2010) examined measures of practice quality for 10,408 physicians in Massachusetts. She found that younger physicians excel in providing acute care — the kind we saw measured in the big outcomes studies I reviewed — and that older physicians do better with preventative care. These measures are just proxies of how well a physician’s patients do and they can’t tell us directly about patients’ actual outcomes. But they suggest the potential for less easily noticed risks associated with younger physicians.
Is it being out of touch with evidence?
The pace of clinical research has been accelerating for some time, which makes it hard for physicians to keep up to date. Many physicians also carry forward practices that they learned during their training, some of which are inevitably found to be ineffectual or even harmful. If older physicians don’t adapt to the new set of best practices — this failure to adapt is sometimes called cognitive inertia — their patients are likely to do worse than those of physicians who were trained on the newer practices.
A 2005 review found evidence of an inverse relationship between age and clinical knowledge across every study that measured that relationship. The studies it cites are decently sized for the most part, with one reporting over 3,300 respondents. They cover a range of both general and disease-specific knowledge. The review also looked at a number of studies examining diagnostic, screening, and preventative practices, about three quarters of which reported that older physicians actually outperform younger physicians — especially interesting in light of the Orler study above. That ratio reverses in the studies looking at appropriate use of therapies: three quarters report that younger physicians outperform their older colleagues.
Evidence in the past couple decades has been relatively scarce on clinical knowledge among older physicians, but the wider availability of clinical and billing data for research purposes has opened the door to examining physician practices change over time in response to evidence. For instance, a 2021 study looked at fibrate prescribing patterns after a study found that adding these lipid-lowering drugs to statin therapy added no additional protection against heart attack in diabetic patients. They didn’t examine age closely, but found no significant difference in the rate of deprescribing between physicians younger than 50 or 50 plus.
Another study published in 2019 traced the declining use of episiotomy as evidence accumulated that it provided no benefit during most births. They found that episiotomy rates dropped over the twenty years it took for this evidence to become robust enough for broad acceptance, but that older physicians were always more likely to perform the procedure: “A 10-year difference in physician age is associated with a 6 percentage point increase in episiotomy rates.”
These studies both focus on abstaining from or subtracting interventions rather than adding them. The evidence in these two cases also seems to have come about in different ways: the fibrate study was a single definitive event, while the evidence against episiotomy built up over decades. This suggests that older physicians might be more likely to change their practices in response to evidence that suddenly overturns standard practice rather than when that happens gradually.
Is it cognitive decline?
Physicians’ cognitive decline with age follows the same general pattern as the public’s but at a slightly slower rate. A period of slow decline appears after age 40, followed by a more rapid loss of cognitive ability after age 60. It’s worth noting, though, that variance in cognitive ability also increases with age — some people maintain a youthful sharpness into old age, even as their peers decline. A skewed distribution of decline could mean that, even if a relatively small number of physicians had substantial cognitive decline, they could bring down the average patient outcomes for everyone in their age group.
While the plot of cognitive ability above might account for the sharp worsening of outcomes among physicians 60+ years old, the notable decline in cognitive test results between 40 and 60 year olds doesn’t match the very small differences in patient outcomes seen for example in the Tsugawa study for this age group. A very small study that looked at tests of clinical competence versus cognitive ability supports the idea that cognitive decline is not the sole source of diminishing patient outcomes among older physicians. This study found that the inverse relationship between clinical competence and age was strengthened when they looked only at respondents with minimal cognitive decline. This suggests that impairment can’t explain the loss of clinical competence.
As we consider whether the evidence on physician age and patient outcomes is attributable to cognitive decline, we need to account for the faculties most likely to decline with age: specifically, fluid intelligence and reasoning tend to falter with age, whereas crystallized intelligence remains intact. This matches a pattern seen in at least one study that analyzed patient encounters with physicians of various ages. It found that the older physicians tended to interrupt their patients more often and to prematurely foreclose diagnostic possibilities before complete investigation. This suggests that the older physicians rely much more on pattern recognition for diagnosis versus seeing diagnosis as a process of hypothesis testing.
Unresolved questions
The evidence on the effect of physician age on patient outcomes raises at least as many questions as it answers. I see the following as important areas of further research:
Are there secular trends in the relationship between age and safety? The rate of aging has been slowing, especially for wealthy white-collar professionals like physicians. This suggests that the conclusions drawn about, say, 60-year-old physicians a couple decades ago might no longer be true. It might be that the non-linear effect of age doesn’t really kick in now until after 65 or 70. There just isn’t enough information to even guess about this at present.
What is the role of technology in promoting high-quality patient care among physicians of all ages? Electronic health record systems now include interactive decision support and are especially vigilant about practices that are included in quality measures and merit-based incentive payments. We might expect that technology — separate from changes in the rate of aging — promotes improved outcomes (or at least intermediate proxies of outcomes) among older physicians.
Is there a differential relationship between aging and stopping practices versus starting novel practices? The evidence on reaction to emerging evidence is largely based on abstaining from procedures or deprescribing medications whose use is no longer evidence-based. There are differences that can speculatively be tied to how the evidence on these practices changed. But I wonder whether it holds for the addition of new practices rather than just their subtraction.
Conclusion
The evidence is reasonably strong that older physicians with low patient volumes produce worse outcomes in inpatient settings. The source of this deficiency isn’t clear. If I had to guess, though, I would speculate that most of the difference is based on lack of information on up-to-date practices, likely exacerbated by smaller patient volumes as physicians age — for instance, as part of a shift towards administrative jobs. A portion of the difference in patient outcomes between younger and older physicians is probably played by cognitive decline, but I suspect that the impact of this is concentrated in a relatively small share of older physicians.
Based on all the evidence, we have to be careful not to extrapolate our conclusions too broadly. For one, there is clearly strong individual variation in ability, rate of aging, training, work experience, and continuous learning that affect a physician’s ability to produce good patient outcomes. Proxies of quality care suggest too that older physicians largely follow guidelines for chronic disease management and preventative care at least as well as younger physicians and possibly even better. Ultimately, my hope is that this evidence is strengthened such that it allows physicians of all ages to practice in settings that match well with their strengths.
Number needed to harm = 1 / (0.121 - 0.108)
There was a small but significant difference for physicians aged 40-49.